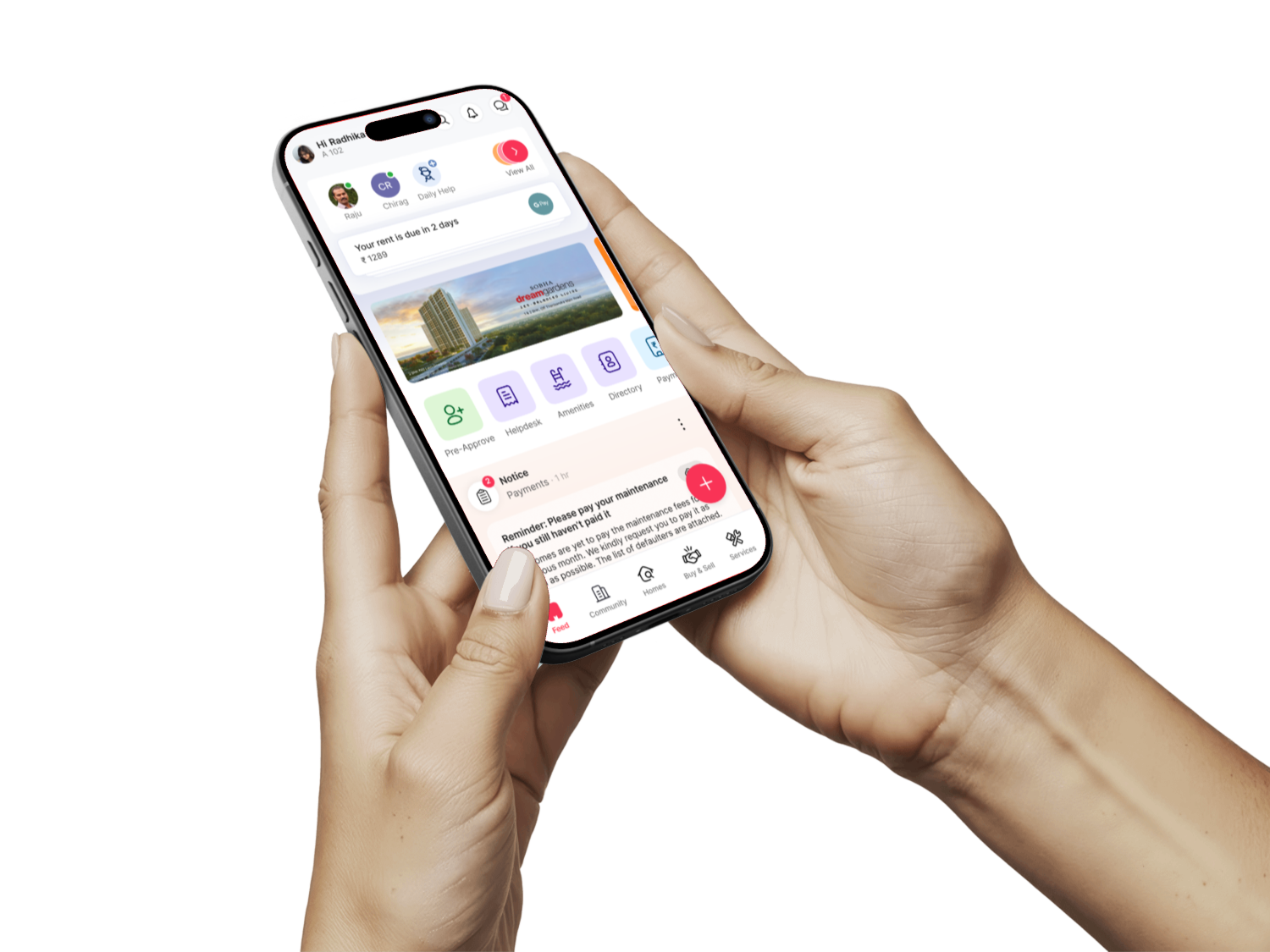
Launched a first-of-its-kind cashless health insurance product at ACKO.
Making cashless insurance work for everyone - at any hospital.
My goal was to create an exceptional insurance experience for all customers at ACKO - making cashless coverage available at both network and non-network hospitals, and building an independent claims processing network to improve efficiency and satisfaction.
While TPAs (Third-Party Administrators) provide a wide hospital network, the overall experience consistently fell short. NPS for cashless claims lagged behind reimbursements by 10%, and processing costs were 65% higher than in-house handling.
The core problem: customers prefer cashless to avoid upfront costs and distrust the reimbursement process - but the existing cashless system at ACKO was slow, expensive, and out of our direct control.
So we asked: what if ACKO took ownership of the cashless process end-to-end, starting with planned hospitalisations?
Why the existing cashless system wasn't working.
We explored alternatives to TPAs for claims processing. Despite their wide network, TPAs fell short across TAT, customer experience, and technology - and came at a significant cost premium.
ACKO was paying ₹1,650 per cashless claim via TPAs, compared to ₹1,000–1,100 in-house - a gap that scaled into crores annually. Meanwhile, cashless NPS was 10% below reimbursement NPS.
Customer interviews and claim data revealed that the preference for cashless wasn't about convenience alone - it was rooted in anxiety. Patients facing hospitalisation didn't want to arrange large sums upfront or trust that reimbursements would arrive in time.
What the data and discovery surfaced.
ACKO's cashless claims data, combined with customer interviews and TPA performance audits, pointed to four interconnected problem areas:
Reasons for Cashless Preference
- Avoiding large upfront costs at non-network hospitals
- Low trust in the reimbursement process
- Fear of delayed or disputed settlements
- Familiarity from corporate policy holders
- High volume of planned hospitalisations
Challenges with TPAs
- Poor TAT and lengthy pre-authorisation
- Limited technology capabilities
- NPS 10% below reimbursement claims
- Cost premium of ~₹650 per claim
- No real-time visibility for customers
Long Wait Times
- 50% of customers wait 30+ minutes for approval
- 25% wait more than 2 hours
- Anxiety amplified during active hospitalisation
High Average Claim Size
- ACS for cashless is 20–30% higher than reimbursements
- Reduced price sensitivity when patients pay nothing upfront
From this, two clear objectives emerged:
Enhance Customer Wait Times
With 50% of users waiting 30+ minutes and 25% over 2 hours, we aimed to slash pre-authorisation friction through a streamlined, app-first approval flow with real-time status.
Improve Average Claim Size (ACS)
By introducing cost visibility and better pre-approval controls, we aimed to reduce claim inflation - without compromising the customer experience during a stressful hospitalisation.
Advance Cash - ACKO takes the wheel on cashless.
We focused on planned hospitalisations first - 30% of cashless claims - with a ₹1 lakh budget cap. With 24×7 support, this model could eventually cover ~50% of all claims in-house.
End-to-end flow from notification to settlement.
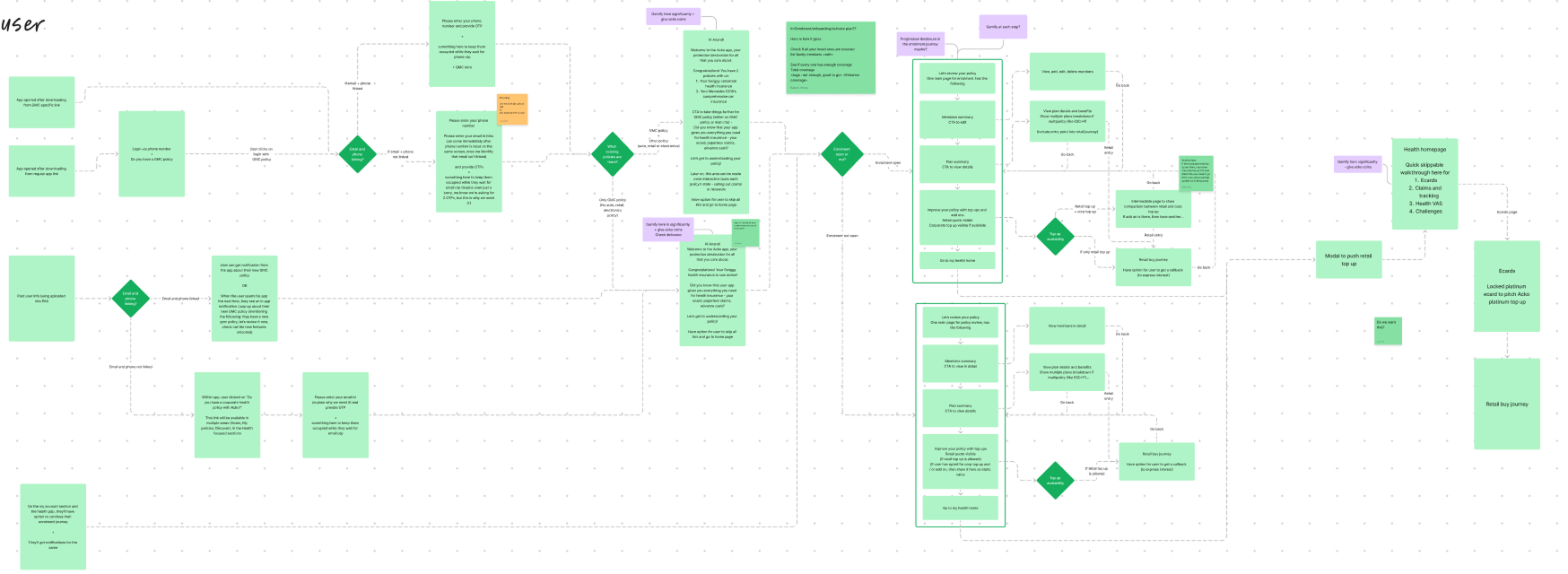
Exploring the structure before visual design.
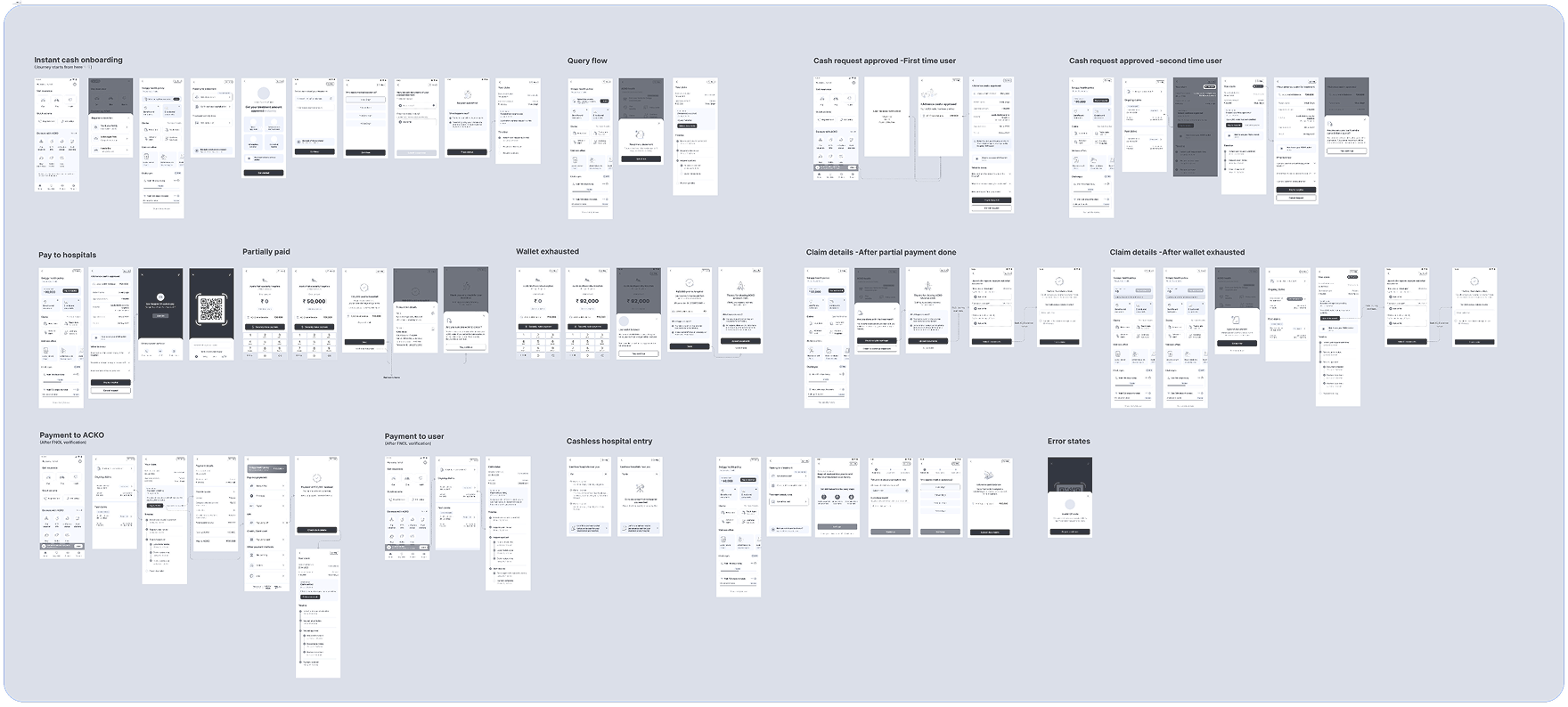
"When you remove the fear of upfront costs, customers don't just trust the product - they trust the brand. Cashless isn't a feature, it's a promise."
The finished product, shipped to corporate customers.
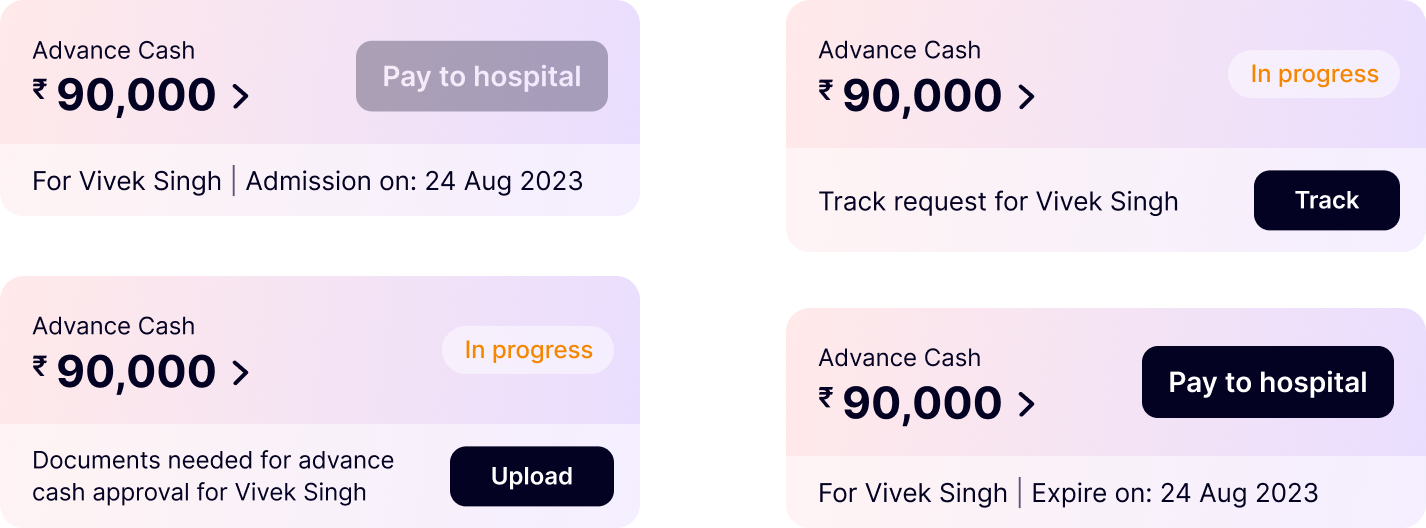
A specialized wallet card on the health home page centralizes all Advance Cash activity - from initiating requests to tracking approvals and making hospital payments - in a single, scannable entry point.
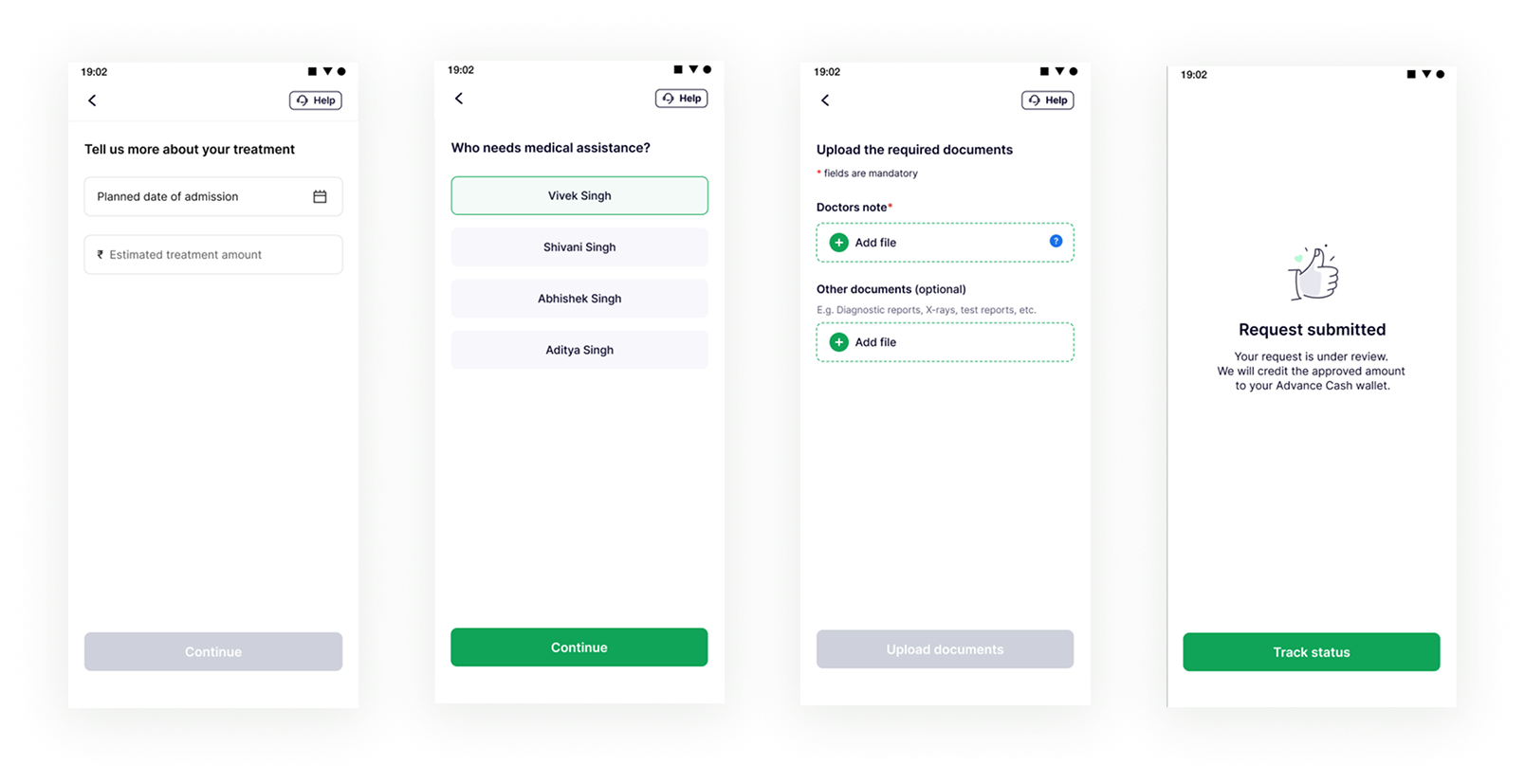
Simplified Advance Cash Requests: Just three steps. Upload your doctor's note. Get your funds. Easy and efficient.
Advance Cash is now accessible through multiple entry points - the App home, Health home, and during the claim process. A dedicated introduction page gives users a clear overview of the feature, including a side-by-side comparison between cashless and advance cash to help them understand which option suits their situation.

The Advance Cash Details page provides users with an overview of how long they can access this feature and their remaining balance. It also serves as an entry point to close the feature when the wallet is fully exhausted.
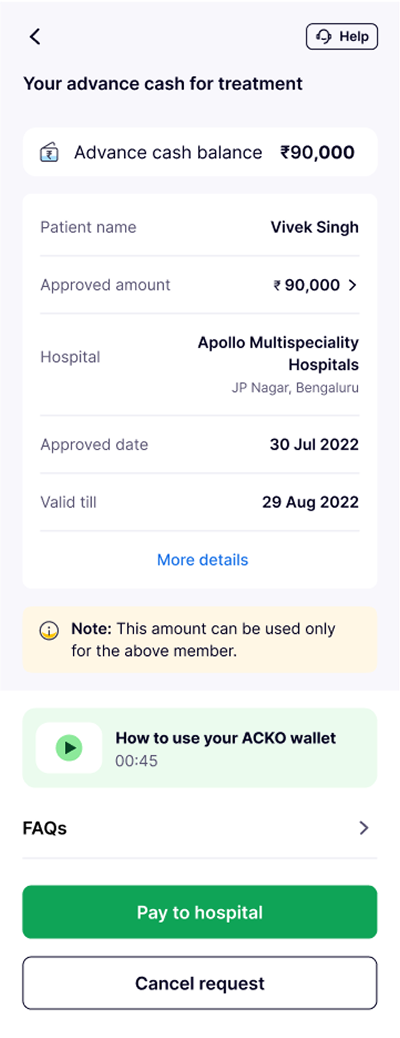
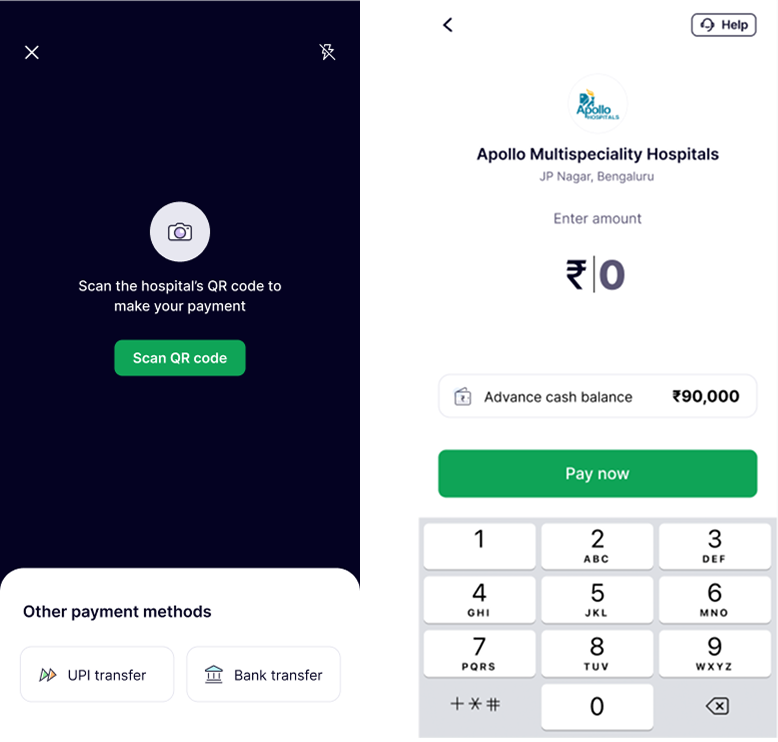
Once funds are in the wallet, users can pay hospitals directly - by scanning, transferring to a UPI ID, or via bank account. Multiple payment modes reduce friction at the most critical point of a hospital visit.
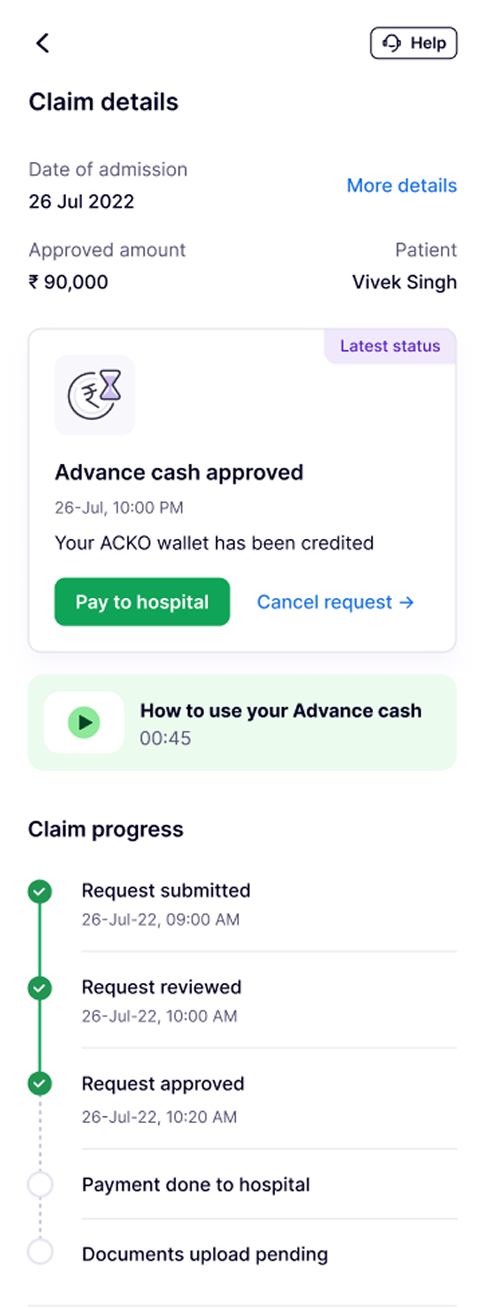
The Claim Details Page serves as a central hub for accessing information regarding claim status and advance cash details. It provides convenient entry points for making direct payments to hospitals through the Claim detail card.
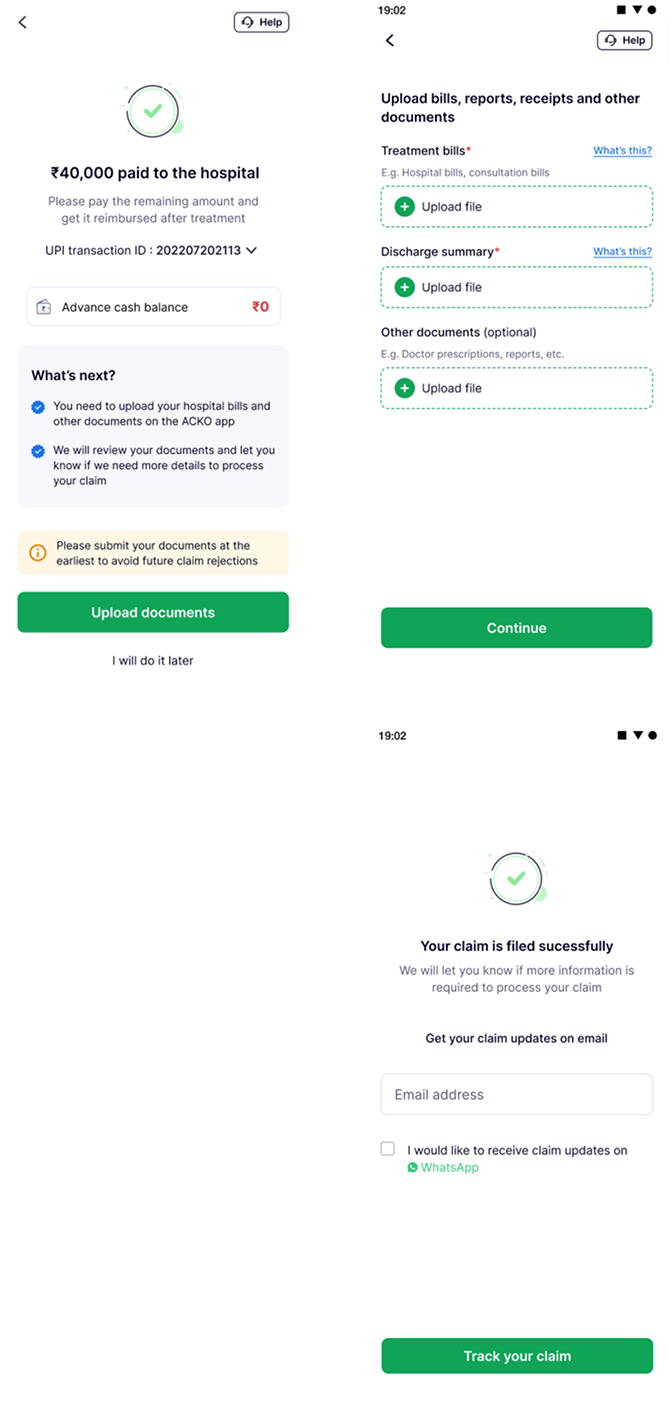
Once all funds are exhausted, users close out the advance cash cycle by uploading their medical records - completing the loop from request to settlement.
Launched to corporate customers - and it worked.
The feature is launched to corporate policy customers in the pilot phase. The initial impact was positive with engagement metrics showing 4,653 users checked this feature.
"The highest approved claim was ₹1,20,000 - with ₹80,000 released. Monthly active usage in May–June was 25 users, growing month-on-month as word spread within corporate cohorts."
"Designing for healthcare means designing for anxiety. Every delay, every unclear status, every extra step compounds the stress of an already difficult moment. Speed and transparency aren't nice-to-haves - they're the product."